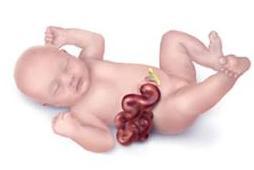
Gastroschisis is a hole in the abdominal wall, which allows a baby’s intestines to protrude outside of the abdominal cavity. Gastroschisis is almost always located immediately to the right of the insertion of the umbilical cord. The hole can also be much larger, which may also cause the stomach, liver or other organs to be exposed.
What causes it?
In most babies, the cause of gastroschisis is unknown. However, recent research has indicated that certain factors can increase the likelihood of having a baby with the condition. Those factors include young mothers (under 20 years of age) and smoking tobacco, drinking alcohol or using recreational drugs during pregnancy.
There are also reports that gastroschisis can occur again within the same family. Some research estimates that gastroschisis can recur in future pregnancies about 4% of the time.
Diagnosis
Most cases of gastroschisis are diagnosed during routine ultrasounds. In addition, second trimester maternal serum alpha–fetoprotein (MSAFP) screening has shown a connection between elevated MSAFP levels and gastroschisis. The diagnosis of abdominal wall defects during the first trimester is difficult because it is normal for the bowel to protrude or push into the base of the umbilical cord. This is why the most reliable ultrasounds occur after 14 weeks of pregnancy, when the bowel should be entirely enclosed in the abdomen.
Treatment Options
Gastroschisis is treated with surgery after birth, at which time the intestines are placed back in the baby’s belly. There are no fetal interventions available at this time.
The extent of surgery required for your baby depends on how much of the intestines or additional organs lie outside of his or her body at birth and if there is an associated atresia or blockage in the intestine. There are 2 main approaches for closure of gastroschisis; primary repair, where the protruded organs are returned to the abdomen and the muscle closed. The alternative approach is delayed closure after placement of the organs in a pre-formed silp bag.
Babies with gastroschisis often need additional treatment during this process, including:
- Intravenous nutritional supplementation
- Antibiotics to prevent infection
- Careful body temperature monitoring
*diagnostic information provided courtesy of our partners at Colorado Fetal Care Center
Read more about Gastroschisis:
Logan’s Recovery from Gastroschisis
The Fetal Health Foundation is a parent-founded non profit helping families experiencing a fetal syndrome diagnosis.
