Talitha A. McGuinness, Fetal Health Foundation Executive Director shares the basics on maternal fetal medicine.
Each summer, millions of expectant parents celebrate the imminent arrival of their new family members with baby showers and parties. In fact, nearly 4 million babies were born in the United States in 2018, the most recent year for which the CDC has published data. Unfortunately, in some pregnancies, the joy that expectant parents feel is often tampered by medical complications and concerns.
Pregnancy complications
The leading causes of high-risk pregnancies include preeclampsia, gestational diabetes, and fetal syndromes. According to the CDC, congenital abnormalities, which fall within the category of fetal syndromes classify a pregnancy as “high risk” and are the #1 cause of death in US infants. More than 800,000 pregnancies are affected by one of 4,000 known fetal syndromes each year. The causes are largely unknown. 6-8% of all pregnancies in the US are characterized as high risk, meaning that there is a serious anomaly that may affect the life of the baby during pregnancy or soon after birth.
Fetal syndromes
Women typically have an ultrasound scheduled around their fifth month into the pregnancy (20 weeks of gestation). This scan serves several purposes, including learning the baby’s gender, but also helps the doctor detect abnormalities with blood flow, and organ and bone development, to name a few areas of interest. But17-24 weeks’ gestation is when fetal syndromes are generally detected.
The Fetal Health Foundation, a national non-profit focused on supporting patient families faced with a fetal syndrome diagnosis, is the only group known to have built an online repository of fetal syndromes, including diagnosis information, possible treatment and outcomes, as well as an interactive map for locating fetal centers that provide syndrome-specific care.
Fetal syndromes include Twin to Twin Transfusion Syndrome, Amniotic Bands, Hydrops and many more.
Maternal Fetal Care Centers
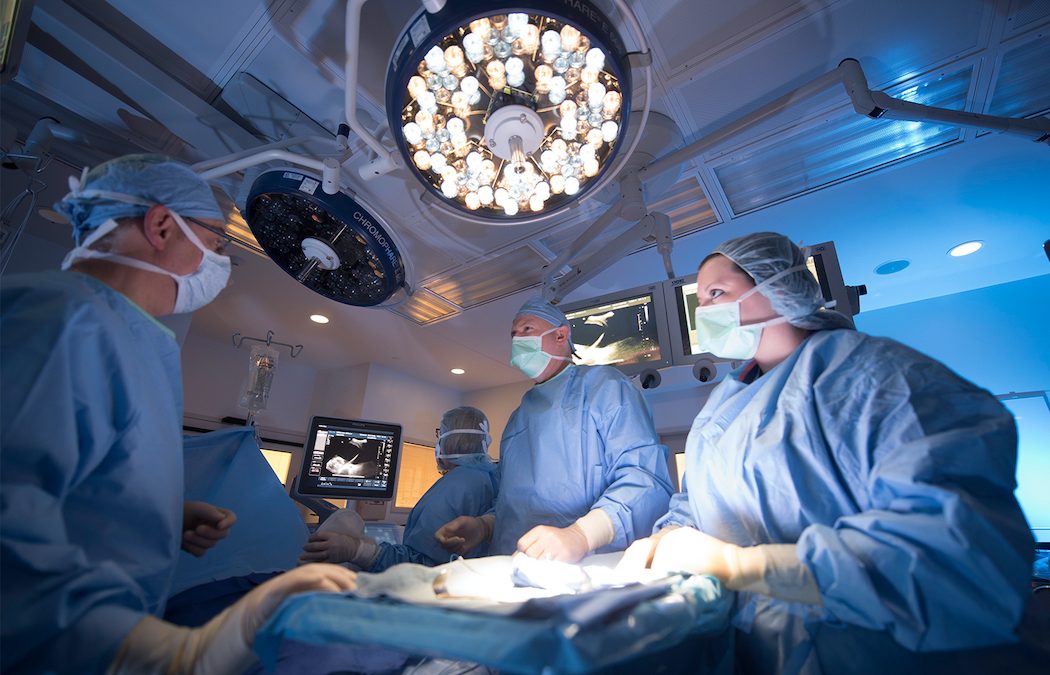
Enter Maternal Fetal Care Centers, where moms and babies alike can be provided with the best care possible. While most babies are delivered and receive the necessary care in the maternity ward at a local hospital, babies that are diagnosed with a fetal health syndrome require special care. Maternal Fetal Care Centers provide specialized and coordinated care for both mother and baby before, during and after complicated pregnancies.
Typically, these centers are staffed by a team of specialists including:
- Maternal-fetal medicine (MFM) specialists: obstetrician/gynecologists with additional training in maternal and fetal complications of pregnancy
- Neonatologists: doctors with expertise caring for newborns with birth defects or complications associated with prematurity
- Board-certified pediatric medical and surgical sub-specialists
“Maternal fetal care centers provide a framework for multi-specialist collaboration in the diagnosis and novel treatments of both mother and baby. This gives hope to families as they manage during this most difficult time in their lives,”said Mary Beth Martin, VP of Women’s and Children’s Services, Doernbecher Children’s Hospital and Fetal Health Foundation Founding Board Member.
Additionally, Maternal Fetal Care Centers have specialized equipment and tools that allow them to treat fetal heath syndromes in a variety of ways, depending on the diagnosis and severity of the individual case, including but not limited to:
- Expectant Management (frequent ultrasound assessments)
- Interventional medications
- Amniocentesis
- Open fetal and minimally invasive surgery
Fetal Surgery
Fetal surgery is a highly complex surgical intervention to mitigate birth defects while babies are still in the womb. It allows doctors to treat serious and life-threatening conditions and stop progressive damage, while also keeping the baby in utero long enough to grow and develop.
The first successful human fetal surgery case was performed in 1981 at the University of California, San Francisco. Since then, more than 5,000 fetal surgeries have been performed worldwide and procedures are being improved upon and developed annually. Today, there are more than two dozen fetal treatment centers in the US alone, many conducting research in fetal medicine, with nearly 80% having just emerged within the last 10 years. Often opened under the umbrella of a children’s hospital, fetal therapy is recognized as one of the most promising fields in pediatric medicine, and prenatal surgery is becoming a viable and much-needed option for a growing number of babies with birth defects. These surgeries and treatment options give patient families tangible hope to fulfill milestones and dreams of having a family, while giving their babies a greater chance at life.
About the Fetal Health Foundation
The Fetal Health Foundation (FHF) is a national nonprofit focused on empowering and supporting expectant parents by providing information, access to world class maternal fetal medical experts, financial support, connections, and counseling. In addition, FHF funds research, increases awareness, and serves as an outlet for leading medical information pertaining to fetal conditions and syndromes.
Photo used with permission by Midwest Fetal Care Center, a collaboration of Allina Health and Children’s Minnesota