Omphalocele affects 1 in 5,000 births. Our thanks to our stewardship partners the UC Davis Fetal Care team for sharing this story of hope with us. We’re delighted to see Everly’s progress.
When Brianne Jacobsen was 20 weeks pregnant, her ultrasound revealed that her developing baby’s internal organs were sticking out of its abdomen. The birth defect, known as an omphalocele, required the higher level of expertise of the UC Davis Fetal Care and Treatment Center team.
Omphaloceles occur in about one out of every 5,000 births. Jacobson’s daughter Everly was that one. Since it cannot be repaired until after the baby’s birth, Jacobsen’s medical team followed her through her pregnancy and were prepared for her child’s delivery.
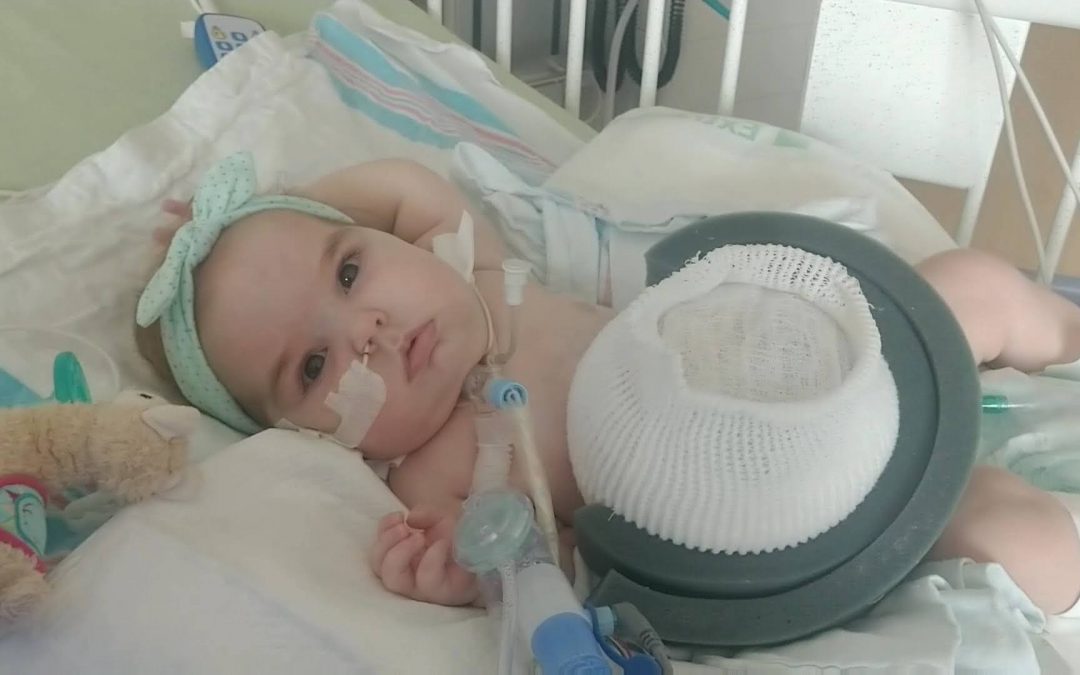
Everly was born full-term in February 2020. Her organs, covered in a thin, transparent skin, were larger than her head and continued to grow. It was classified as a giant omphalocele. At its peak, it was larger than her entire torso. Giant omphaloceles are associated with high mortality rates and a high risk of severe morbidity.
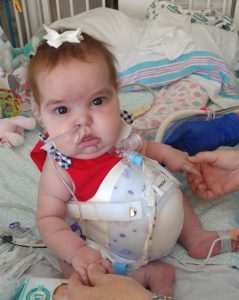
“Everly had one of the largest omphaloceles that many of us had ever seen,” said Robyn Huey Lao, pediatric surgery outpatient nurse practitioner at UC Davis Health. “But Everly’s skin tissue was also abnormal.”
Huey Lao said for patients with an omphalocele, treatment usually involves the use of silver sulfadiazine cream, which is used to treat second- and third-degree burns and toughens the skin. Then the organs are compressed back into the abdominal cavity. The medical team typically waits until the child is older before planning a surgical closure.
“But hers remained very delicate and pliable. We couldn’t safely compress it,” she added.
A life-saving surgical repair
As her liver, intestines and other organs were outside of Everly’s abdomen, protected only by her very pliable skin, it was imperative that the team find a solution.
In the Neonatal Intensive Care Unit (NICU), the clinical nurse specialist and pediatric surgical nurse practitioners tried various treatments, including Medihoney (a medical grade honey product), Mepilex (an absorbent foam dressing) and Triad cream (a Zinc-oxide based paste) to toughen up her skin. They changed her dressings each day and ensured that she would be safe to go home from the hospital.
When Everly was back home and five months old, her omphalocele ruptured. Her organs spilled out of her skin and she was life flighted back to UC Davis Children’s Hospital, where the pediatric surgery team performed a life-saving surgical repair using AlloDerm, a decellularized sterile tissue made from human cadaver skin.
But her skin refused to heal. Huey Lao rose to the challenge, sampling different wound care treatments, hoping that one would work for Everly.
From soccer ball-sized to an outie belly button
After many trials, Huey Lao discovered that Vashe, a solution of hypochlorous acid that cleans wounds, was the right formula, when paired with UrgoTul silver, a flexible, polyester mesh contact layer bandage. Once the skin fully healed over the omphalocele, compression dressings were applied over time to gradually push Everly’s organs back inside.
“Now what was a soccer ball-sized omphalocele is something that looks like an outie belly button,” Jacobsen said. “The transformation has been amazing.”
Her surgeon plans to close up the opening in her abdominal wall this summer, the final chapter in what has been a long journey for her family since her birth. Everly is now 2 ½ years old.
Improving health outcomes for Everly
Since the omphalocele has been compressed, the family has seen positive changes in her.
When Everly was five months old, the ear, nose and throat team performed a tracheostomy, a surgical hole made in the front of the neck and into the windpipe, with assisted ventilation to help her breathe. While she used to be dependent on the ventilator for 24 hours a day, she has slowly weaned off of oxygen and can now spend 75 to 80% of her time off of the ventilator.
Now she can eat and drink normally, when once she relied on a nasogastric tube (NG tube), a special tube that carries food and medicine to the stomach through the nose.
When Everly was born, she had severe pulmonary hypertension (PH), a type of high blood pressure that occurs in the arteries of the lungs, associated with her omphalocele and incomplete lung development. The multidisciplinary pediatric pulmonary hypertension team aggressively treated her PH to optimize lung growth. The team has seen her PH remain stable on their therapies, despite the internalization of her omphalocele, which puts external pressure on her lungs. They continue to monitor her in their clinic.
Now, Everly can run on the playground, unencumbered. It’s something that wasn’t possible with a giant omphalocele a year ago.
“We are excited and amazed we’ve come this far from where we started. If I could hand out Daisy Awards, I would give them to her doctors and nurses, who have become life-long friends,” said Jacobsen, who moved their family to Sacramento last year from Redding to be closer to UC Davis Children’s Hospital. “They didn’t just care for my daughter. They took care of me and Everly’s dad. They’re a big part of Everly’s success and our confidence as parents. We are so grateful to this team for everything they have done for her and for us.”
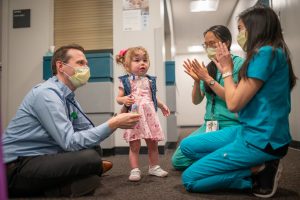
2-year-old fetal surgery patient Everly Jacobsen meeting with her care team including NP Robyn Huey Lao and the pulmonary hypertension team of Dr. Brian Goudy, Dr. Rory Kamerman-Kretzmer and nurse practioner Callie Brecek. Mom is Breanne