
by Erika K Wolf | Dec 11, 2025 | Blogs, Condition, Fetal Hydrops, front-page, Myelomeningocele/Spina Bifida, News, Spina Bifida, Story
When Taylor and James learned their baby, Rose, had spina bifida, their world shifted overnight. From high-risk pregnancy care to in-utero surgery at Children’s Mercy, their story of hope, resilience, and the power of compassionate medical support unfolded.

by Erika K Wolf | Oct 9, 2025 | Blogs, Condition, front-page, Myelomeningocele/Spina Bifida, News, Spina Bifida, Story
Dr. Diana Farmer of UC Davis is pioneering new spina bifida treatments by combining fetal surgery with stem cell therapy in the groundbreaking CuRe Trial. Her work is transforming patient care and offering hope.

by Erika K Wolf | Dec 3, 2024 | Blogs, Condition, front-page, Myelomeningocele/Spina Bifida, News, Spina Bifida, Story, Uncategorized
5-minute read
Ester and Samuel traveled across country and stayed away from home for months to ensure the health of their baby boy. His serious spina bifida diagnosis and mom’s cervical complications were challenges that Dr. Timothy Crombleholme accepted and triumphed over.

by Erika K Wolf | Oct 29, 2024 | Blogs, Condition, front-page, Myelomeningocele/Spina Bifida, News, Spina Bifida, Story, Uncategorized
The landmark clinical trial CuRe Trial: Cellular Therapy for In Utero Repair of Myelomeningocele is underway at UC Davis Health. The world’s first spina bifida treatment combining fetal surgery with stem cells could change the life of a baby with spina bifida, who could otherwise be paralyzed from the waist down.

by Erika K Wolf | Oct 28, 2024 | Blogs, Condition, front-page, Myelomeningocele/Spina Bifida, News, Spina Bifida, Story
Christian was the 14th patient to undergo fetal surgery for myelomeningocele, a severe form of spina bifida, at Children’s Hospital of Philadelphia. He is now a tall, handsome 24-year-old who recently passed his national certification to become an emergency medical technician (EMT).
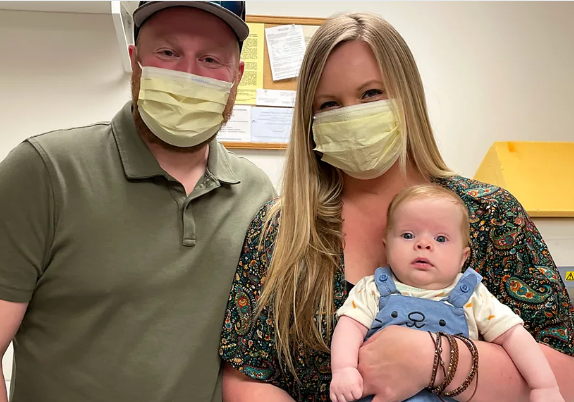
by Erika K Wolf | Oct 28, 2024 | Blogs, Condition, front-page, Myelomeningocele/Spina Bifida, News, Story
Oregon couple traveled to California for in-utero surgery at nearly 26 weeks gestation to repair the baby’s spina bifida defect. During the operation, doctors placed a stem cell patch on the baby’s small spine. The results are making waves around the world.






